AI medical billing market to reach $45Bn by 2035: Precedence Research
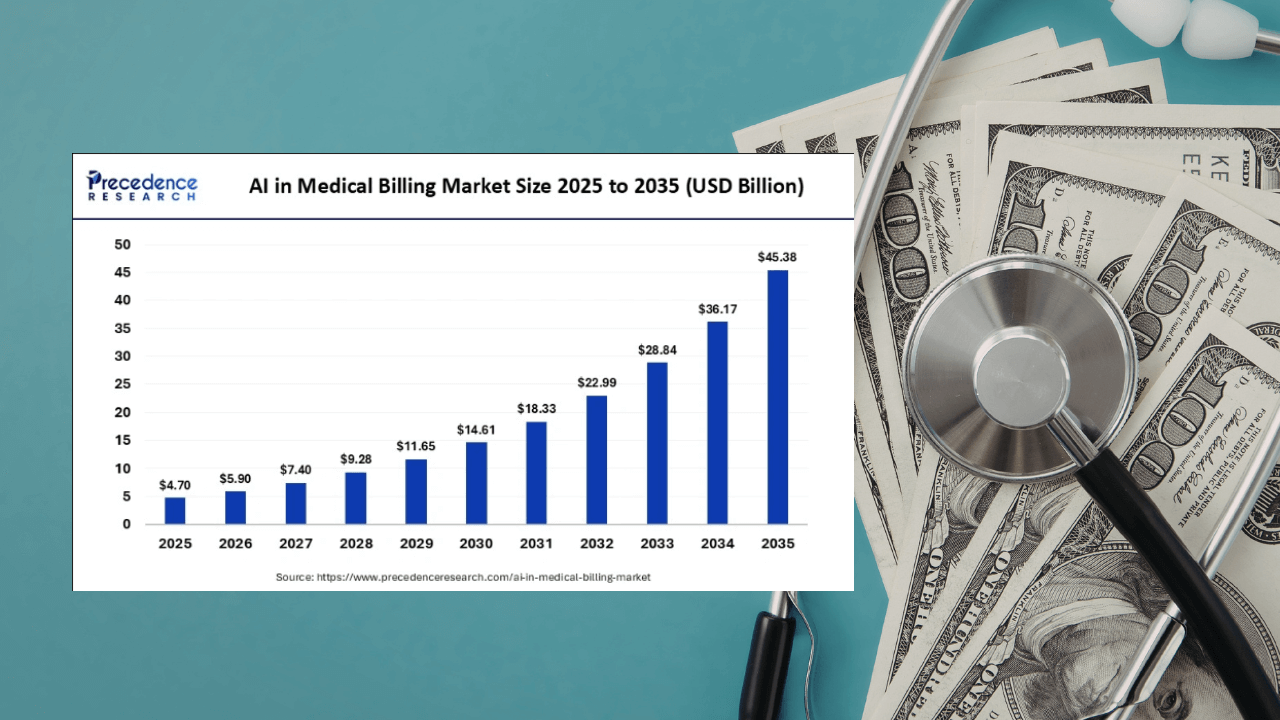
ONTARIO, CANADA — The global market for AI-powered medical billing is set for a dramatic surge, projected to leap from US$5.9 billion in 2026 to US$45.38 billion by 2035 with a compound annual growth rate (CAGR) of 25.44%, according to a new market projection by Precedence Research.
This rapid growth is fueled by healthcare providers’ increasing reliance on artificial intelligence (AI) to reduce billing errors, accelerate claims processing, and improve financial performance.
The shift is expected to reshape not only domestic healthcare operations but also the demand for offshore medical coding and revenue cycle management (RCM) services.
How AI technologies reshape medical billing and coding
AI technologies — including machine learning, natural language processing, and predictive analytics — have become essential for the automating of medical billing systems.
“The global AI in medical billing market includes artificial intelligence-powered platforms and services used to automate healthcare billing processes such as medical coding, claim submission, denial management, RCM, and payment processing,” the report stated.
Market trends demonstrate that cloud-based platforms have become the dominant solution since 2025, as these platforms provide businesses with scalable, flexible, and cost-effective solutions.
The fastest growth of hybrid deployments will enable organizations to store their sensitive patient and financial data on local systems while they use AI-driven analytics.
Key industry players are establishing strategic alliances to combine AI technology with their current billing knowledge. Google Cloud partnered with IKS Health to enhance coding and prior authorization workflows, which shows how AI technology is increasingly being integrated into RCM operations.
Impact of AI on medical billing outsourcing and RCM
The expansion of AI in medical billing is expected to significantly impact offshore billing, coding, and RCM providers.
“The billing outsourcing firms segment is expected to expand at the highest CAGR during the forecast period. The market growth of this segment is because outsourcing companies are quickly adopting AI technologies to increase efficiency and expand their business with multiple healthcare clients,” the study noted.
For outsourcing firms, AI offers a dual opportunity: to enhance operational efficiency through automation and to broaden service offerings across the global healthcare market.
Hospitals and clinics that make up 56% of the market in 2025 use AI technology for coding, claim denial management, and revenue cycle optimization. This allows offshore providers to implement these solutions, which enable them to process claims at large volumes while achieving higher accuracy and faster processing times.
The trend could redefine outsourcing roles, with AI handling routine coding while human expertise focuses on complex claims, audits, and compliance, creating a more strategic, high-value role for offshore teams.
The medical billing industry is undergoing its first major transformation as North American and Asia Pacific countries and other territories are experiencing a rapid increase in their adoption of AI technology.
Offshore medical coding and RCM services have become the focal point of a global effort to achieve better healthcare system administration through automated processes that utilize AI technology.

 Independent
Independent




